
A golden era of antibiotics shifted the leading causes of death away from infection to cancer and cardiovascular disease. At the moment, we can still treat most infections as only a few are resistant to the last line of antibiotics (currently the colistins) – but history shows us this will change and it is changing as we speak as colistin resistance grows in China and now in the US.
While prizes are being awarded for new research to combat resistance, farmers are slammed for overuse of antibiotics in livestock, doctors chided for unnecessary prescriptions and pharmaceutical companies criticised for a lack of investment in favour of more profitable drugs.
Meanwhile new antibiotic discoveries are rare if not non-existant and exciting new methods aren’t seen by many as enough to avert doomsday. Some believe technology – and even older ways – might save us. Others have already laid out what we need to do now to save ourselves while we still can.
We aren’t in the post-antibiotic era yet, but we are in danger of getting there fast – and it could be worse than the pre-antibiotic era.
So what would the world be like if no antibiotics were available? We only have to go back 70 years, before the “golden era” of antibiotic discoveries of the 1940s to 1960s, to experience infectious disease as the predominant cause of human death. These diseases are still around and some are more virulent – now complicated by multiple antibiotic resistances, which evolved through many factors, but mostly driven by our overuse.

City life: up close and personal.
However, society has also changed since the days before antibiotics. There are more of us and we live closer together as cities grow and populations move in from rural areas. We also live in a cleaner society which, ironically, some say makes us more vulnerable to disease.
New diseases (and some that have re-emerged) have also had significant impact in the past couple of decades: Legionnaires disease, Lyme disease and Weil’s disease, highly pathogenic E. coli (usually a friend that lives in our colon, but can become our worst enemy). These will inevitably become more antibiotic resistant with time.
Without antibiotics some old, established diseases that don’t hit our current top worst ten will start return as silent assassins. Our dogged foe, tuberculosis, will rise immeasurably. Pneumonia will once again become a mass-killer, particularly among the old and frail – and maybe everyone else too.
Bigger risk.
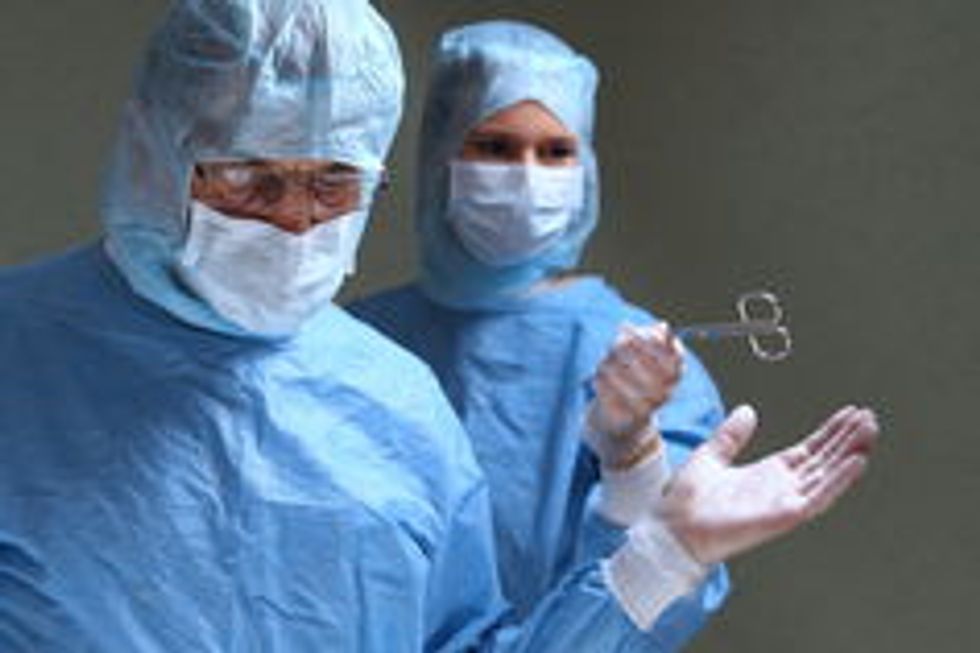
Transplant surgery would become virtually impossible as the immuno-suppressing drugs that are essential to our bodies accepting the transplants leave us unable to fight off life-threatening infections without antibiotics. Even removing a burst appendix would be a dangerous operation once again, as all operations become life threatening if septicaemia takes its toll unimpeded.
Dogged resistance
Ironically, we wouldn’t worry about antibiotic resistance anymore – no antibiotics would be prescribed because they wouldn’t work. It is a mainstay of the argument against resistance that the use of fewer antibiotics will reduce resistance.
Resistance is driven by the presence of antibiotics causing mutation and resistance genes to flow between pathogens (and non-pathogens). Resistance in some cases makes the pathogen stronger. If you reduce this selection, you reduce resistance in these strains too. But if we imagined that completely taking away antibiotics would do away with resistance altogether and create a world where we could start using them again, we’d be wrong.
Let’s put aside the argument that millions, maybe billions, of people who would die if antibiotics weren’t used anymore because the same prediction holds if we continue to apply ineffective antibiotics. Resistance still wouldn’t disappear completely as a small reservoir of genes would be maintained in natural bacterial populations. Just when it was safe to use antibiotics again, resistance would return, but probably at a quicker rate as it has already been established. The soil, water, in fact the environment as a whole will always remain a reservoir for resistance, ready to be spread and make our antibiotics ineffective again.
Post-antibiotic dystopia
So how would society change in a post-antibiotic era? Will we still greet people with a hug or handshake, or keep each other at arm’s length and view them with suspicion? Will we travel by aircraft, that tube of recirculating air and a known route for global spread of infections? Will we even want to use the train, the bus or the car? Will we always wear masks or develop biological containment suits (one for every occasion)? Will protective segregation occur between the fit and the less fit that alters societal structures? Will we think twice about pastimes that may harm us? Or will we be inventive and unite with global policies against a common enemy, invest and find new antimicrobials, develop new therapies or apply a combination of all these strategies?
The sentiments of physiologist Kevin Fong ring out:
If we are to avoid a return to the pre-antibiotic landscape with all its excess mortality we must be bold. To squander the advantage we have so recently gained against microorganisms in the fight for life would be unthinkable.
Slowly but surely a worldwide realisation is emerging that this is not a rehearsal and we are past the opening night. National governments are starting to look for solutions but are having to balance their energies against other threats like the Zika virus. Regardless, from government to citizen, we have to take notice. Perhaps we (and all governments) should read the ten solutions offered up by Jim O'Neill in a UK report and do something about it before it is too late.
![]()
Roger Pickup, Professor of Environment and Human Health, Lancaster University
This article was originally published on The Conversation. Read the original article.





